Graft Survival Rates: Factors Affecting Procedure Outcomes
Understanding graft survival rates is essential for anyone considering a hair restoration procedure. The success of hair transplantation depends heavily on how well transplanted follicles adapt to their new location. Multiple biological, technical, and post-operative factors influence whether grafts thrive or fail. This article examines the key elements that determine graft survival, explores different transplantation methods, and provides insights into costs and patient suitability for those seeking effective solutions to hair loss.
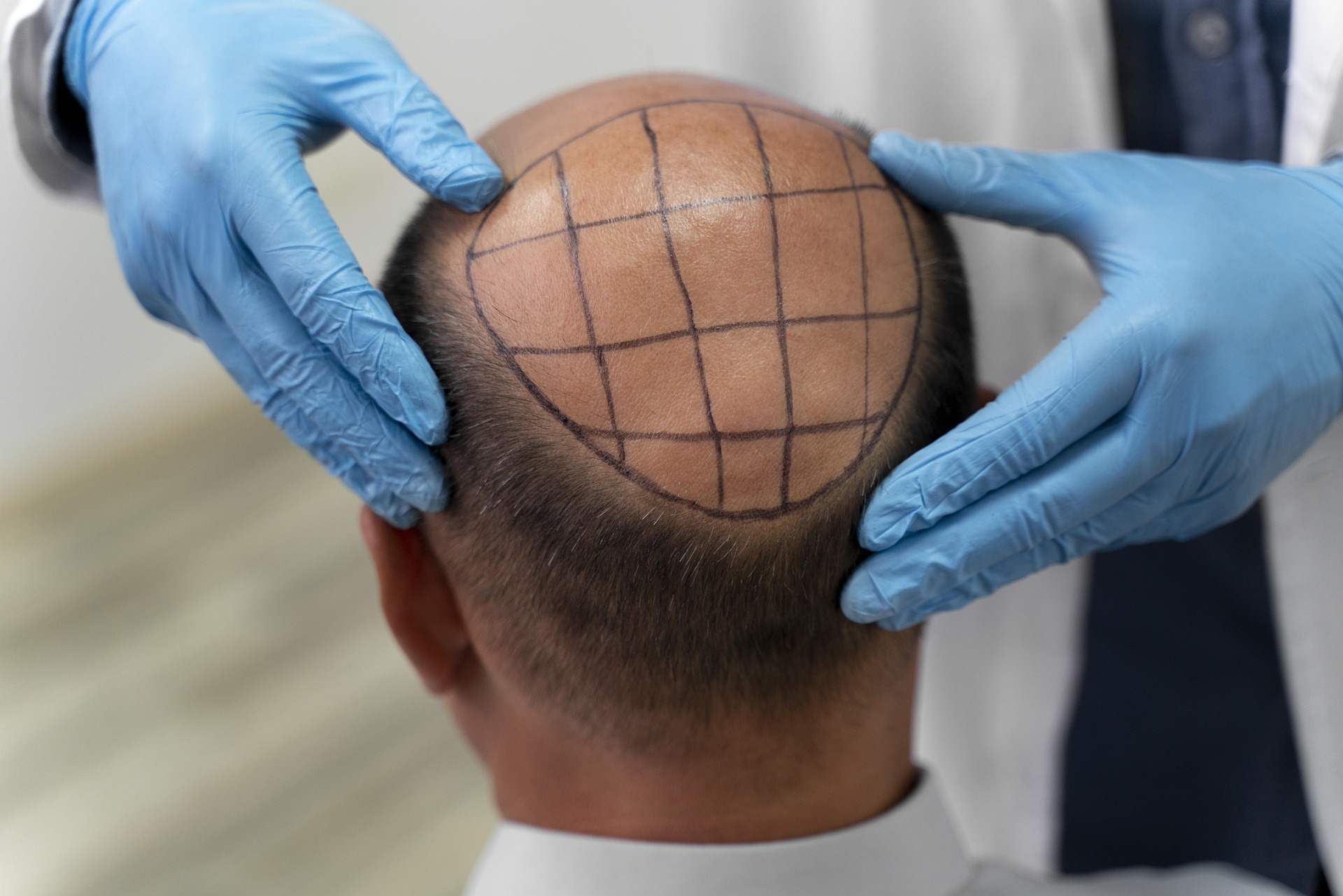
Graft survival is the cornerstone of successful hair restoration. When follicular units are extracted and relocated, their ability to establish blood supply and continue growing determines the overall outcome. Studies indicate that survival rates typically range from 85% to 95% in well-executed procedures, though individual results vary based on numerous factors including surgical technique, patient health, and aftercare adherence.
What Determines Graft Survival After Transplantation
Several critical factors influence whether transplanted hair follicles survive and produce lasting results. The time grafts spend outside the body significantly impacts viability—follicles kept in specialized storage solutions maintain better integrity than those exposed to air for extended periods. Surgeon skill plays an equally important role, as precise extraction and implantation minimize trauma to delicate follicular structures. Patient-specific factors such as scalp blood circulation, overall health status, and genetic predisposition to healing also contribute substantially to survival rates. Additionally, the angle and depth of graft placement affect how quickly follicles receive nutrients from surrounding tissue.
Understanding Different Hair Transplantation Methods
Two primary techniques dominate modern hair restoration: Follicular Unit Transplantation (FUT) and Follicular Unit Extraction (FUE). FUT involves removing a strip of scalp from the donor area, dissecting it into individual grafts, and implanting them in recipient zones. This method allows harvesting large numbers of grafts in a single session but leaves a linear scar. FUE extracts individual follicular units directly from the scalp using specialized punches, leaving tiny circular scars that heal less visibly. A newer variation, Direct Hair Implantation (DHI), uses a pen-like device to insert grafts immediately after extraction, reducing handling time and potentially improving survival rates. Each method has distinct advantages depending on patient needs, hair characteristics, and desired coverage area.
How Follicles Are Transplanted and Handled During Surgery
The transplantation process begins with donor area preparation, typically the back or sides of the scalp where hair is genetically resistant to thinning. After local anesthesia, surgeons extract grafts using their chosen method while maintaining follicle integrity. Extracted grafts are immediately placed in chilled storage solutions containing nutrients and growth factors that preserve cellular function. Technicians examine each graft under magnification, trimming excess tissue while protecting the bulb and dermal papilla—the structures essential for hair growth. Recipient sites are created at precise angles matching natural hair direction, and grafts are carefully inserted to ensure proper depth and orientation. The entire process requires meticulous attention to minimize trauma and maximize survival potential.
Who Benefits Most From Hair Restoration Procedures
Ideal candidates for hair transplantation typically experience pattern baldness with sufficient donor hair density. Men with male pattern baldness (androgenetic alopecia) and women with diffuse thinning in specific areas often achieve excellent results. Younger patients should demonstrate stable hair loss patterns, as progressive thinning may require additional procedures later. Medical evaluation helps identify individuals whose hair loss stems from treatable conditions rather than genetic factors—thyroid disorders, nutritional deficiencies, or autoimmune conditions may require alternative treatments. Patients with realistic expectations, good overall health, and adequate donor reserves generally experience the highest satisfaction rates. Those with certain scalp conditions, bleeding disorders, or unrealistic density expectations may not be suitable candidates.
Cost Considerations and Pricing Factors in Germany
Hair transplantation costs in Germany vary considerably based on technique, clinic reputation, and the number of grafts required. Understanding these financial aspects helps patients make informed decisions about their treatment options.
| Procedure Type | Typical Cost Range | Grafts Included |
|---|---|---|
| FUE (Small Session) | €2,500 - €5,000 | 1,000 - 2,000 grafts |
| FUE (Large Session) | €5,000 - €10,000 | 2,000 - 4,000 grafts |
| FUT (Strip Method) | €3,000 - €7,000 | 2,000 - 3,500 grafts |
| DHI (Direct Implantation) | €4,000 - €12,000 | 1,500 - 3,000 grafts |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Cost per graft typically decreases with larger sessions, though total expenses increase proportionally. Premium clinics with experienced surgeons and advanced technology charge higher rates but often deliver superior graft survival and aesthetic outcomes. Geographic location within Germany also affects pricing, with major cities like Berlin, Munich, and Frankfurt generally commanding higher fees than smaller regional centers. Additional expenses may include pre-operative consultations, post-operative medications, follow-up appointments, and potential touch-up procedures. Some clinics offer financing options or package deals that include accommodation for international patients.
Post-Operative Care and Long-Term Graft Survival
The critical period for graft survival extends approximately two weeks after surgery, during which follicles establish new blood supply. Patients must avoid physical activities that increase blood pressure, refrain from touching or scratching the scalp, and follow prescribed washing protocols carefully. Sleeping with the head elevated reduces swelling and prevents graft displacement. Most transplanted hairs shed within the first month—a normal process called shock loss—before entering a resting phase. New growth typically begins three to four months post-surgery, with significant improvement visible by eight to twelve months. Full results emerge after 12 to 18 months as transplanted follicles complete their growth cycles. Long-term survival depends on maintaining scalp health through proper nutrition, stress management, and potentially using medications like finasteride or minoxidil to preserve existing hair.
Successful hair restoration combines surgical expertise, appropriate technique selection, and diligent aftercare. While graft survival rates remain high with modern methods, individual outcomes depend on multiple interacting factors. Patients considering these procedures should consult qualified specialists, understand realistic expectations, and commit to post-operative protocols that maximize their investment in renewed confidence and appearance.




